Connect With Us
Featured Articles

What is a Plantar Wart?
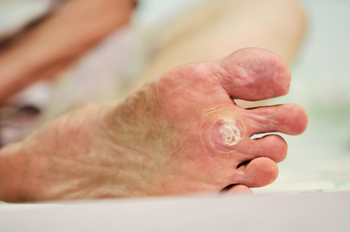 The location for plantar warts to develop is on the heel of the foot. The wart will typically grow into the foot as a result of the constant pressure the feet endure by standing, walking or running for the majority of the day. They are known to be caused by the human papillomavirus, which is also referred to as HPV, and is considered to be the most common viral infection of the skin. This particular virus can enter the body through small cuts on the bottom of the foot, and it often thrives in moist and warm areas. People who frequently swim in pools or use public showers may be prone to contracting plantar warts. There are symptoms indicative of plantar warts, and these may include severe pain and discomfort while walking, standing or running, in addition to small black dots appearing in the center of the wart. If you have developed a plantar wart, please consult with a podiatrist for the best treatment techniques for you.
The location for plantar warts to develop is on the heel of the foot. The wart will typically grow into the foot as a result of the constant pressure the feet endure by standing, walking or running for the majority of the day. They are known to be caused by the human papillomavirus, which is also referred to as HPV, and is considered to be the most common viral infection of the skin. This particular virus can enter the body through small cuts on the bottom of the foot, and it often thrives in moist and warm areas. People who frequently swim in pools or use public showers may be prone to contracting plantar warts. There are symptoms indicative of plantar warts, and these may include severe pain and discomfort while walking, standing or running, in addition to small black dots appearing in the center of the wart. If you have developed a plantar wart, please consult with a podiatrist for the best treatment techniques for you.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Dr. Rouder from S.I. Podiatry. Our doctor will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
- Lesions on the bottom of your feet, usually rough and grainy
- Hard or thick callused spots
- Wart seeds, which are small clotted blood vessels that look like little black spots
- Pain, discomfort, or tenderness of your feet when walking or standing
Treatment
- Freezing
- Electric tool removal
- Laser Treatment
- Topical Creams (prescription only)
- Over-the-counter medications
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact our office located in Staten Island, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar Warts
Plantar warts are growths that typically appear on the heels or other weight-bearing areas of the feet. These warts are caused by the human papillomavirus (HPV). The virus enters the body through breaks in the skin, such as cuts, that are on the bottom of the feet. Plantar warts are more likely to affect children and teenagers, people with weakened immune systems, people who have a history with plantar warts, and people who walk barefoot in environments exposed to a wart-causing virus.
If you suspect you have plantar warts, you may have the following symptoms: pain or tenderness while walking, a lesion that interrupts the ridges in the skin of your foot, small fleshy lesions on the bottom of the foot, or a callus where a wart has grown inward over a well-defined spot on the skin.
HPV causes plantar warts to form and is very common. There are more than 100 kinds of the virus in existence. However, only a few of them cause warts on the feet. The other types of HPV are likely to cause warts on other parts of the body.
If you have plantar warts, your podiatrist may try different treatment methods depending on your specific case. Some treatments for plantar warts are peeling medicines (salicylic acid), freezing medicines (cryotherapy), or surgical procedures. Laser treatments and vaccines are also used to treat plantar warts.
Three Common Foot Disorders

Bunions, plantar fasciitis, and Morton’s neuroma are common foot disorders that cause pain and difficulty walking. A bunion occurs when the big toe deviates from the smaller toes, creating a bony bump at the base of the joint. A podiatrist can recommend modifying footwear, using orthotic devices, or, in persistent cases, performing surgery to correct the deformity. Plantar fasciitis, a painful inflammation of the connective tissue along the bottom of the foot, often causes heel pain, especially after periods of rest. Treatment includes stretching, wearing supportive footwear, orthotic inserts, or surgery, if symptoms remain after more conservative care. Morton’s neuroma involves thickening of nerve tissue between the toes, often leading to burning pain or numbness in the ball of the foot. A podiatrist may suggest shoe modifications, metatarsal pads, or carefully considered injections. If necessary, surgery may be needed to remove the affected nerve. If you regularly experience foot pain, it is suggested that you schedule an appointment with a podiatrist for a diagnosis and appropriate treatment.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Dr. Rouder from S.I. Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact our office located in Staten Island, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Foot Pain
The feet, being the foundation of the body, carry all of the body’s weight and are therefore prone to experiencing pain and discomfort. If you are experiencing foot pain, it is important to determine where in the foot you are experiencing this pain to help discover the cause of it. While pain can be experienced virtually anywhere in the foot, the most common sites of foot pain are in the heel and ankle.
Heel pain can be due to a multitude of conditions including plantar fasciitis, Achilles tendinitis, and heel spurs. Pain experienced in the ankle can be a sign of an ankle sprain, arthritis, gout, ankle instability, ankle fracture, or nerve compression. In more serious cases, pain in the foot can be a sign of improper alignment or an infection.
Foot pain can be accompanied by symptoms including redness, swelling, stiffness and warmth in the affected area. Whether the pain can be described as sharp or dull depends on the foot condition behind it. It is important to visit your local podiatrist if your foot pain and its accompanying symptoms persist and do not improve over time.
Depending on the location and condition of your foot pain, your podiatrist may prescribe certain treatments. These treatments can include but are not limited to prescription or over-the-counter drugs and medications, certain therapies, cortisone injections, or surgery.
If you are experiencing persistent foot pain, it is important to consult with your foot and ankle doctor to determine the cause and location. He or she will then prescribe the best treatment for you. While milder cases of foot pain may respond well to rest and at-home treatments, more serious cases may take some time to fully recover.
What Is an Ankle Fracture?

Ankle fractures occur when one or more of the bones in the ankle joint break, often caused by a fall, twisting injury, or sports-related impact. Common symptoms include sharp pain, swelling, bruising, and difficulty bearing weight or moving the ankle. The treatment approach depends on the severity of the fracture. For mild cases, rest, elevation, and immobilization with a cast or splint may be enough. More serious fractures, especially those involving misaligned bones, often require surgery using pins, plates, or screws to stabilize the joint and promote healing. After initial treatment, guided exercises may be recommended to restore strength, flexibility, and mobility. Follow-up care is essential to monitor healing and avoid long-term issues like joint stiffness or instability. A podiatrist can provide an accurate diagnosis, treatment options, and a recovery plan. If you think you may have fractured your ankle, it is suggested that you make an immediate appointment with a podiatrist.
Broken ankles need immediate treatment. If you are seeking treatment, contact Dr. Rouder from S.I. Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Broken Ankles
A broken ankle is experienced when a person fractures their tibia or fibula in the lower leg and ankle area. Both of these bones are attached at the bottom of the leg and combine to form what we know to be our ankle.
When a physician is referring to a break of the ankle, he or she is usually referring to a break in the area where the tibia and fibula are joined to create our ankle joint. Ankles are more prone to fractures because the ankle is an area that suffers a lot of pressure and stress. There are some obvious signs when a person experiences a fractured ankle, and the following symptoms may be present.
Symptoms of a Fractured Ankle
- Excessive pain when the area is touched or when any pressure is placed on the ankle
- Swelling around the area
- Bruising of the area
- Area appears to be deformed
If you suspect an ankle fracture, it is recommended to seek treatment as soon as possible. The sooner you have your podiatrist diagnose the fracture, the quicker you’ll be on the way towards recovery.
If you have any questions, please feel free to contact our office located in Staten Island, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
All About Broken Ankles
Broken ankles are a serious injury that can lead to an inability to walk, function, and also cause a significant amount of pain. A broken ankle is a break in one of the three bones in your body that connect at the ankle joint: the tibia, the fibula, and the talus. The tibia and fibula are your two primary leg bones that connect at the knee, which sit directly upon the talus bone. This is protected by a fibrous membrane that allows for movement in the ankle joint. A broken ankle is usually caused by the foot rolling under or twisting too far, causing one of these three bones to snap.
A broken ankle is different from an ankle sprain, which occurs when the ankle ligaments are ripped or torn but no bones have been broken. A sprain can still be very severe, causing bruising in the foot and an inability to hold your own weight, much like a broken ankle would. If you’re unable to stand, and suspect that you have a broken ankle, the first thing to do would be to get an immediate X-ray to determine the severity of the break.
A common cause of broken ankles is when the ankle is rolled over with enough pressure to break the bones. This usually happens during exercise, sports, or other physical activity. Another common cause is a fall or jump from a tall height.
One immediate treatment for pain relief is elevating the foot above your head to reduce blood flow to the injured area. You can also apply ice packs to your ankle to help reduce swelling, redness, inflammation, and pain. After these initial steps, getting a cast and staying off your feet as much as possible will aid in the recovery of the broken ankle. The less movement and stress the ankle has to endure, the more complete it will heal. A doctor can determine if surgery is needed in order to heal correctly. In these cases, an operation may be the only option to ensure the ability to walk properly again, followed by physical therapy and rehabilitation.
It is highly important to determine if surgery is needed early on, because a broken ankle can become much more severe than you realize. If not professionally treated, the broken ankle will inhibit your walking, daily functioning, and produce a large amount of pain. Treating your broken ankle early on will help prevent further damage to it.
Why Live with Pain and Numbness in Your Feet?
Understanding Hammertoe
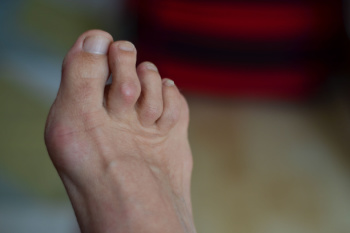
Hammertoe is a foot deformity in which one or more of the smaller toes bend abnormally at the middle joint, creating a curled or hammer-like appearance. This condition often develops gradually and can become rigid over time if not treated. Common causes include an imbalance in the muscles or tendons that control toe movement, often triggered by wearing tight or ill-fitting shoes that crowd the toes. Repeated pressure and friction can worsen the deformity. Risk factors include having a longer second toe, certain inherited foot structures, or conditions such as arthritis and diabetes. Wearing high heels or shoes with narrow toe boxes may also increase the likelihood of developing hammertoe. If you have signs of hammertoe, it is suggested that you are under the care of a podiatrist who can offer effective relief and treatment methods.
Hammertoe
Hammertoes can be a painful condition to live with. For more information, contact Dr. Rouder from S.I. Podiatry. Our doctor will answer any of your foot- and ankle-related questions.
Hammertoe is a foot deformity that affects the joints of the second, third, fourth, or fifth toes of your feet. It is a painful foot condition in which these toes curl and arch up, which can often lead to pain when wearing footwear.
Symptoms
- Pain in the affected toes
- Development of corns or calluses due to friction
- Inflammation
- Redness
- Contracture of the toes
Causes
Genetics – People who are genetically predisposed to hammertoe are often more susceptible
Arthritis – Because arthritis affects the joints in your toes, further deformities stemming from arthritis can occur
Trauma – Direct trauma to the toes could potentially lead to hammertoe
Ill-fitting shoes – Undue pressure on the front of the toes from ill-fitting shoes can potentially lead to the development of hammertoe
Treatment
Orthotics – Custom made inserts can be used to help relieve pressure placed on the toes and therefore relieve some of the pain associated with it
Medications – Oral medications such as anti-inflammatories or NSAIDs could be used to treat the pain and inflammation hammertoes causes. Injections of corticosteroids are also sometimes used
Surgery – In more severe cases where the hammertoes have become more rigid, foot surgery is a potential option
If you have any questions please contact our office located in Staten Island, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Hammertoe
Hammertoe is a foot deformity that occurs due to an imbalance in the tendons, muscles, or ligaments that are responsible for holding the toes in their normal position. This condition may be caused by poor footwear, foot structure, trauma, and disease. The most common solution for hammertoe is to relieve the pain by changing your footwear and wearing orthotics. In severe cases, surgery may be required.
The shoes that are most likely to cause hammertoe are high heeled shoes or shoes that are too tight in the toe box. Tight shoes will force your toes to crowd together in a curled position. This position will likely continue when you take your shoes off. Another cause is trauma. When you stub your toe, you are increasing the chance that you will develop hammertoe.
There are risk factors that may make you more likely to develop this condition. Women are more likely to have the condition compared to men, and it is also more likely to appear in those who are older in age.
Many different foot problems can be avoided by wearing shoes that have adjustability, adequate toe room, and low heels. Furthermore, if you want to buy new shoes, you should look to purchase them at the end of the day and make sure you know your correct size. The importance of buying shoes at the end of the day is that your feet swell as the day progresses. You should also ensure that you are wearing your correct size because your shoe size may change as you grow older.
To diagnose someone with hammertoe, your podiatrist will need to conduct a thorough examination of your foot. Your doctor may even order an x-ray to evaluate the bones and joints of your feet and toes.
If you have hammertoe, your podiatrist may recommend that you wear shoes that fit you better along with inserts to place inside them. Additionally, he or she may suggest special exercises for you to perform to stretch your toes. One helpful exercise it to pick up marbles with your feet or crumple a towel with your toes.
Prior to meeting with your podiatrist, it will be helpful to make a list of all the symptoms you are experiencing. You should also make a note of medications you are taking and important personal information about your medical history.
Causes and Treatment of Toenail Fungus
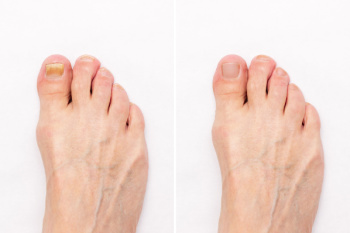
Toenail fungus is an infection that affects the toenail and the skin underneath it. It often causes the nail to become thick, yellow, and brittle, or to lift away from the nail bed. Fungal toenails are more common in older adults, especially those with diabetes, poor circulation, or a weakened immune system. Fungus grows well in warm, damp places like sweaty shoes. For that reason, people who wear tight or closed shoes for long hours or use shared shower areas may be more likely to be exposed. The infection usually starts slowly and can become worse over time if not treated. Because toenails grow slowly and have less blood flow than other parts of the body, treating a fungal nail infection can take several months. A podiatrist may prescribe oral medication to fight the infection from the inside, or use topical treatments for mild cases. In more serious situations, surgery to remove the damaged nail might be recommended. If you have been infected with a toenail fungus, it is suggested that you make an appointment with a podiatrist for treatment.
For more information about treatment, contact Dr. Rouder of S.I. Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please feel free to contact our office located in Staten Island, NY . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.