Connect With Us
Featured Articles

How to Select the Ideal Running Shoe

Choosing the right running shoe is a critical decision that directly impacts both comfort and performance. Different foot types and running styles necessitate a personalized approach to ensure the perfect fit. For those individuals with high arches, cushioned shoes with ample shock absorption help absorb impact and provide essential support. Conversely, individuals with low arches or flat feet benefit from stability shoes that offer extra arch support and motion control. Runners who overpronate or supinate require shoes designed to address their specific gait patterns, preventing potential injuries. Determining your foot type and understanding your running mechanics are pivotal in guiding the selection process. Ultimately, investing time in finding the right running shoe tailored to your individual needs enhances not only the running experience but also safeguards against potential discomfort and injury. If you would like specific information about how to find the right running shoes for your needs, it is suggested that you consult a podiatrist.
If you are a runner, wearing the right running shoe is essential. For more information, contact Dr. Rouder from S.I. Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Choosing the Right Running Shoe for Your Foot Type
To increase performance and avoid the risk of injury, it is important to choose the right running shoe based on your foot type. The general design of running shoes revolves around pronation, which is how the ankle rolls from outside to inside when the foot strikes the ground.
- Neutral runners are able to choose from a wide variety of shoes, including minimalist shoes or even going barefoot.
- Runners who overpronate, or experience an over-abundance of ankle rolling, should choose shoes that provide extra motion control and stability.
- Runners who underpronate, or supinate, have feet that have high arches and lack flexibility, preventing shock absorption. They require shoes with more flexibility and cushion.
If you have any questions please feel free to contact our office located in Staten Island, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Choosing the Right Running Shoe for Your Foot Type
Running may seem like a simple to do. However, running is actually a complex movement that puts stress on the ligaments, bones, and joints of the body. Selecting the correct running shoe is important for increasing performance and avoiding risk of injury. Running shoes should be selected based on your foot type. Considerations such as trail versus road shoes are important. Your foot type dictates the degree of cushioning, stability and motion control you require. The most accurate way to learn your foot type is to visit a local shop that specializes in running shoes. Professionals can measure your arch type, stride and gait and help you with your shoe needs.
The design of running shoes is created around the idea of pronation. Pronation is the natural rolling movement of your ankle from the outside to inside when your foot strikes the ground. If you run properly you strike the ground on the outside of your heel and roll in the direction of your big toe before pushing off once more. Pronation is beneficial because it assists the lower half of your body in absorbing shock and storing energy. Those considered neutral runners pronate correctly and do not need running shoes that help correct their form. Neutral runners can choose from a wide variety of shoes, including barefoot or minimal types. However, those who have arch problems or who adopt an incorrect form while running may experience too much or too little pronation. They may require running shoes that offer additional support.
Those who overpronate experience an over-abundance of ankle rolling. Even while standing, those who severely overpronate display ankles that are angled inward. It is not uncommon for them to have flat feet or curved legs. The tendency to overpronate may cause many injuries. Areas that tend to become injured are the knees, ankles, and Achilles tendon. If you find that you have a tendency to overpronate, you should look at shoes that provide extra stability and motion-control. Motion-control shoes are straight and firm. Shoes of this type do not curve at the tip. The restricted flexibility along the middle of the shoe prohibits the foot from rolling too far inward as your foot strikes the ground.
A less common problem is underpronation. Underpronation, also called supination, is when the feet are unable to roll inward during landing. Those who underpronate have feet that lack flexibility and high arches. This prevents any kind of shock absorption, even though it does place less rotational stress on ankles and knees. This added force can cause fractures, ligament tears, and muscle strains because the legs are trying to compensate for the impact. Those who underpronate need shoes with more cushioning and flexibility. If you have a tendency to underpronate, selecting stability or motion-control shoes may cause you more problems by continuing to prevent pronation.
Arthritis Can Cause Pain in the Feet and Ankles
How Podiatrists Manage Arthritis

Rheumatoid arthritis, or RA, is the most common form of inflammatory arthritis, and it often results in foot-related problems in up to 90 percent of those diagnosed. The foot can be an initial site for RA symptoms, with symptoms that include soreness, swelling, and joint erosion. A podiatrist can identify, diagnose, and treat these foot-related challenges, with an aim to alleviate pain, enhance function, and protect overall foot health. Their palliative foot care includes addressing distorted or altered nails, hard skin, calluses, and corns. A podiatrist also specializes in wound management, offering timely interventions for wounds and ulcers on the feet as they develop. Custom orthotics, ranging from soft cushions to firmer devices, can improve foot alignment and function. A podiatrist can contribute to joint protection, manage inflamed joints, suggest appropriate exercises, and provide insights into surgical options when necessary. Their comprehensive care extends beyond immediate foot concerns, aiming to enhance overall foot health and contribute to the well-being of those navigating the challenges of rheumatoid arthritis. For more information about managing foot problems associated with RA, it is suggested that you include a podiatrist as a permanent member of your medical team.
If you are experiencing pain in the feet or ankles, don’t join the stubborn majority refusing treatment. Feel free to contact Dr. Rouder from S.I. Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Podiatrist?
Someone would seek the care of a podiatrist if they have suffered a foot injury or have common foot ailments such as heal spurs, bunions, arch problems, deformities, ingrown toenails, corns, foot and ankle problems, etc.
Podiatric Treatment
A podiatrist will treat the problematic areas of the feet, ankle or lower leg by prescribing the following:
- Physical therapy
- Drugs
- Orthotic inserts or soles
- Surgery on lower extremity fractures
A common podiatric procedure a podiatrist will use is a scanner or force plate which will allow the podiatrist to know the designs of orthotics. Patients are then told to follow a series of tasks to complete the treatment. The computer will scan the foot a see which areas show weight distribution and pressure points. The podiatrist will read the analysis and then determine which treatment plans are available.
If you have any questions please feel free to contact our office located in Staten Island, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
What is a Podiatrist?
The branch of medicine that is focused on the treatment, diagnosis, and study of disorders of the lower leg, ankle and foot is referred to as podiatry. Because people often spend a great deal of their time on their feet, many problems in this area can occur. A person seeks help from the field of podiatry when they need treatment for heel spurs, bunions, arch problems, deformities, ingrown toenails, corns, foot and ankle problems, infections, and problems with the foot that are related to diabetes and additional diseases.
To treat problems of the foot, ankle or lower leg, a podiatrist may prescribe physical therapy, drugs, perform surgery, or set fractures. Individuals may also be recommended to wear corrective shoe inserts, custom-made shoes, plaster casts and strappings in order to correct deformities.
When trying to gather information on a patient problem, a scanner or force plate may be used in order to design orthotics. During this procedure, patients are told to walk across a plate that is connected to a computer; the computer then takes a scan of the foot and indicates weight distribution and pressure points. The computer readouts will give the podiatrist information to help them determine the correct treatment plans.
Diagnosis is also provided through laboratory tests and x-rays. Through the foot, the first signs of serious problems such as heart disease, diabetes and arthritis can show up. For example, individuals that have diabetes may frequently have problems such as infections and foot ulcers because they experience poor circulation in the foot area. A podiatrist can then have consultations with patients when symptoms arise. Referrals will then be made to specialists that handle the greater health problems.
Some podiatrists have their own independent, private practices or clinics where they have a small staff and administrative personnel. Many podiatrists work within group practices. They usually spend time performing surgery in ambulatory surgical centers or hospitals, or visit patients in nursing homes. Podiatrists typically spend between 30 to 60 hours of week working. Some podiatrists specialize in public health, orthopedics, surgery, or primary care. Other fields include specialties in geriatrics, dermatology, pediatrics, diabetic foot care and sports medicine.
Some podiatrist specialists complete extra training in the area of foot and ankle reconstruction that results from the effects of physical trauma or diabetes. There are also surgeons that perform surgery of a cosmetic nature to correct bunions and hammertoes.
Symptoms and Causes of Poor Circulation in the Feet
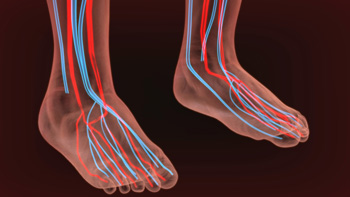
Poor circulation in the feet is a condition where blood flow to the lower extremities is compromised, leading to various symptoms and potential health risks. One of the most common symptoms of poor circulation in the feet is persistent coldness, even when the weather is warm. Numbness and tingling sensations can also occur, making it uncomfortable to stand or walk. Swelling in the feet and ankles is another sign, as restricted blood flow can lead to fluid buildup. This condition can cause the feet to appear pale or bluish in color, and wounds or sores may take longer to heal. Muscle cramps and chronic foot pain, particularly during physical activity, can also be indicators of poor circulation. Several factors can contribute to poor circulation in the feet. Peripheral artery disease, or PAD, is a common cause, where atherosclerosis narrows the arteries and reduces blood flow. Conditions like diabetes can damage blood vessels, while smoking and obesity also can strain circulation. High blood pressure, a sedentary lifestyle, and blood clots can also hinder blood flow. If you have symptoms of poor circulation in your feet, it is suggested that you schedule an appointment with a podiatrist to identify the cause. Once that is determined, the proper treatment can be given for effective management and prevention of complications.
While poor circulation itself isn’t a condition; it is a symptom of another underlying health condition you may have. If you have any concerns with poor circulation in your feet contact Dr. Rouder of S.I. Podiatry. Our doctor will treat your foot and ankle needs.
Poor Circulation in the Feet
Peripheral artery disease (PAD) can potentially lead to poor circulation in the lower extremities. PAD is a condition that causes the blood vessels and arteries to narrow. In a linked condition called atherosclerosis, the arteries stiffen up due to a buildup of plaque in the arteries and blood vessels. These two conditions can cause a decrease in the amount of blood that flows to your extremities, therefore resulting in pain.
Symptoms
Some of the most common symptoms of poor circulation are:
- Numbness
- Tingling
- Throbbing or stinging pain in limbs
- Pain
- Muscle Cramps
Treatment for poor circulation often depends on the underlying condition that causes it. Methods for treatment may include insulin for diabetes, special exercise programs, surgery for varicose veins, or compression socks for swollen legs.
As always, see a podiatrist as he or she will assist in finding a regimen that suits you. A podiatrist can also prescribe you any needed medication.
If you have any questions, please feel free to contact our office located in Staten Island, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Causes Symptoms and Treatment for Poor Circulation in the Feet
The purpose of the body’s circulation system is to transport blood, oxygen, and nutrients throughout the body. A reduction of blood to a specific part of the body may cause one to experience symptoms of poor circulation. The most common causes of poor circulation in the feet are obesity, diabetes, and heart conditions such as peripheral artery disease (PAD). Common symptoms of poor circulation include tingling, numbness, throbbing, pain and muscle cramps.
Peripheral artery disease is a common cause of poor circulation in the legs. Symptoms of PAD are cramping, pain or tiredness in the leg or hip muscles while walking or climbing stairs. This pain tends to go away with rest and starts back up when you begin to walk. It is a condition that causes the blood vessels and arteries to become narrow. Although PAD is more common in adults over the age of 50, it may also occur in younger people. A similar condition called atherosclerosis causes arteries to stiffen up due to a buildup of plaque in the arteries and blood vessels.
Blood clots are also a common cause of poor circulation in the feet. Clots may obstruct blood vessels and if they occur in the legs, they may eventually lead to pain and discoloration. This occurrence is commonly known as deep vein thrombosis (DVT) and it may travel to the lungs. Varicose veins are another condition that may lead to poor circulation, and it is caused by incompetence of the valves in the veins. Women who are overweight are prone to developing this condition. Lastly, diabetes, which is correlated with poor blood sugar metabolism may lead to chronic poor circulation. Those with diabetes often suffer from cramping in the legs, calves, thighs and buttocks.
If you are looking for ways to avoid poor circulation there are some tips you can follow. One tip is to avoid sitting for too long. If you plan to sit down for a long period of time, you should try standing up occasionally, to improve your circulation. Another great way to avoid poor circulation is to exercise. Exercise is an excellent way to pump the heart and increase blood flow. Those who suffer from poor circulation should also avoid smoking, reduce their salt intake, and try to lose weight.
If you are experiencing symptoms from poor circulation in your feet, you should consult with your podiatrist to determine the best method for treatment for you. He or she may prescribe medication in addition to recommending specific lifestyle changes to improve your circulation.
Causes of Peroneal Tendonitis
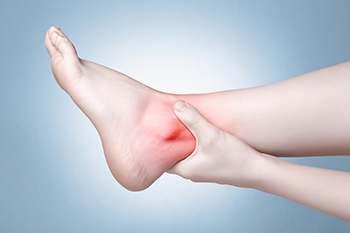
Peroneal tendonitis, a source of pain surrounding the ankle, often targets individuals engaged in rigorous physical activities, particularly runners and athletes who intensify their training routines. This condition typically evolves gradually, progressing from mild discomfort to persistent pain around the ankle. The primary culprit behind peroneal tendonitis is overuse. Sudden spikes in training intensity, coupled with inappropriate footwear or flawed training techniques, frequently trigger this ailment. Sports that demand quick pivoting movements, such as basketball, football, and gymnastics, are particularly associated with the development of tears in the peroneal tendons. Runners who frequently traverse sloped or uneven surfaces, causing the foot to excessively roll out into eversion, face an elevated risk of peroneal tendonitis. Anyone with a history of ankle injuries or recurrent sprains may be more susceptible to peroneal tendon problems. The continuous damage to the ligaments supporting the foot and ankle results in weakened stability, placing increased strain on the peroneal tendons. An abnormal foot position, where the heel is turned slightly inward or if the arch is too high, heightens the risk of peroneal tendonitis. These conditions force the peroneal muscles and tendons to work harder, which contributes to their overuse and potential inflammation. Tight calf muscles combined with weakness in the calf and peroneal muscles may be factors leading to tendonitis. If you are experiencing ankle pain that may be a sign of peroneal tendonitis, it is suggested that you schedule an appointment with a podiatrist for a full exam and diagnosis.
Ankle pain can have many different causes and the pain may potentially be serious. If you have ankle pain, consult with Dr. Rouder from S.I. Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Ankle pain is any condition that causes pain in the ankle. Due to the fact that the ankle consists of tendons, muscles, bones, and ligaments, ankle pain can come from a number of different conditions.
Causes
The most common causes of ankle pain include:
- Types of arthritis (rheumatoid, osteoarthritis, and gout)
- Ankle sprains
- Broken ankles
- Achilles tendinitis
- Achilles tendon rupture
- Stress fractures
- Tarsal tunnel syndrome
- Plantar fasciitis
Symptoms
Symptoms of ankle injury vary based upon the condition. Pain may include general pain and discomfort, swelling, aching, redness, bruising, burning or stabbing sensations, and/or loss of sensation.
Diagnosis
Due to the wide variety of potential causes of ankle pain, podiatrists will utilize a number of different methods to properly diagnose ankle pain. This can include asking for personal and family medical histories and of any recent injuries. Further diagnosis may include sensation tests, a physical examination, and potentially x-rays or other imaging tests.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are rest, ice packs, keeping pressure off the foot, orthotics and braces, medication for inflammation and pain, and surgery.
If you have any questions, please feel free to contact our office located in Staten Island, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Ankle Pain
Pain experienced in the ankle can be caused by a multitude of conditions. While the most common cause is an ankle sprain, other possible problems can include arthritis, gout, ankle instability, an ankle fracture, nerve compression, or tendinitis. In more serious cases, ankle pain can be a sign of improper alignment of the foot or an infection.
Ankle pain can often be accompanied by symptoms such as redness, swelling, stiffness, and warmth in the affected area. Pain can be described differently depending on the condition: short, stabbing pain and a dull ache are some examples. If such symptoms are persistent and do not improve after time, be sure to schedule an appointment with your local podiatrist.
Depending on the condition causing your ankle pain, different treatments may be prescribed by your podiatrist. For ankle sprains, the first step in treatment involves rest, ice, elevation, and compression. Be sure to avoid placing pressure on the ankle, use an ice pack several times a day, and use a compression bandage and elevation to reduce swelling. Other, more serious conditions may require the assistance of certain drugs and medications such as nonsteroidal anti-inflammatory drugs (NSAIDs), physical therapy, or even cortisone injections.
Depending on the severity of your ankle pain and the condition behind it, recovery from ankle pain may take some time.
Consult with your foot and ankle doctor to best determine the cause of your ankle pain and the appropriate treatment.
What Causes Morton’s Neuroma?
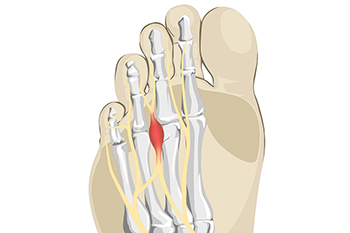
Morton's neuroma is a painful condition that affects the ball of the foot, typically between the third and fourth toes. It is caused by the thickening or enlargement of the tissue around a nerve leading to the toes. Several factors contribute to the development of Morton's neuroma. Wearing tight, narrow, or high-heeled shoes can compress the toes and increase pressure on the nerve, leading to irritation and inflammation. Additionally, individuals with certain foot deformities, such as high arches or flat feet, are more prone to developing Morton's neuroma because these conditions can alter the distribution of weight and pressure on the nerves. Engaging in activities that involve repetitive stress on the forefoot, like running or activities that require tight footwear, can contribute to the development of this condition. A foot injury or trauma can lead to the formation of scar tissue around the nerve, which can then become irritated and inflamed. If you experience symptoms associated with Morton's neuroma, such as pain, numbness, or a burning sensation in the ball of your foot, it is suggested that you schedule an appointment with a podiatrist for a proper diagnosis and treatment.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact Dr. Rouder of S.I. Podiatry. Our doctor will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact our office located in Staten Island, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.